CUES – filling the gaps a year on
23 March 2021

When it was first published, the COVID-19 Urgent eyecare service (CUES) pathway was promoted for the immediate crisis; to help ensure timely access to urgent and emergency eye care in a “COVID-safe” way, without the need to travel to a hospital or, in some cases, even leave home.
However, it was always intended that CUES would also deliver against the NHS long term plan objectives and be a fit for the future, a future without COVID but where urgent eyecare is still delivered locally, optimising the existing workforce across the eye care pathway and reducing the need to travel to a hospital.
The service requires triage and remote consultation at the point of access to help identify patient need so people are seen by the right clinician, in the right place, first time.
Zoe Richmond, LOCSU Interim Clinical Director said: “Within CUES many people aren’t actually ‘seen’ at all but are offered immediate advice and support without the need for a face-to-face appointment. A significant number of people presenting with urgent eye care symptoms are fully managed in this remote way.”
Whilst a number of local systems commissioned and implemented CUES at pace at the start of the pandemic, areas with established Minor Eye Conditions Services (MECS) were able to readily adapt their service specification to support the delivery of urgent eyecare and meet the principles of a CUES service, others have taken a more considered approach and are just beginning to implement CUES, not for the pandemic but as part of a new whole system pathway redesign for the continued delivery of safe urgent eyecare.
Whilst it is not mandatory for CCGs to commission local urgent eyecare services from primary care optometry, commissioning has continued throughout 2020 for example Knowsley CCG are implementing their new service this month and North Cumbria CCG have just announced their intention to commission. This is to meet the eye health needs whilst we continue to work in COVID-safe ways but also to support the much broader aims of the NHS long term plan. Currently 78% CCGs have now commissioned an urgent eye care service from primary care optometry, which means 75% of the population of England now have access to urgent eyecare from their local optometric practice.
Carrie MacEwen, Consultant Ophthalmologist, GIRFT Ophthalmology co-Clinical Lead said: “The transparent demonstration of these data on the availability of urgent eyecare services via CUES and MECS provides an instant understanding of how local systems of care have been and are being rolled across the country. The presence of a CUES/MECS type service is requested as part of the GIRFT ophthalmology review process – looking at variation across regions and systems – and this work helps to illustrate these differences which can be used to explore why they exist.”
LOCSU are working closely with NHS England and Improvement, with the aim to gain a better understanding of whether urgent eyecare provision is in place in the areas without a locally commissioned CUES, if so to understand what this looks like and if not to understand the barriers to commissioning. Early discussions suggest a number of reasons for the lack of commissioning, which include:
- Financial challenges – even where there is clinical consensus that CUES would benefit the system.
- Lack of local engagement – commissioners have other local priorities / limited capacity or just don’t know who to talk to.
- Sufficient capacity – commissioners report adequate provision elsewhere in the system (Hospital Eye Service and / or locally commissioned Community Ophthalmology Services).
- Local resistance – a resistance to change somewhere in the system.
The graphs below show the regional variation across England. This data will allow each NHS region to benchmark itself against the rest of England.
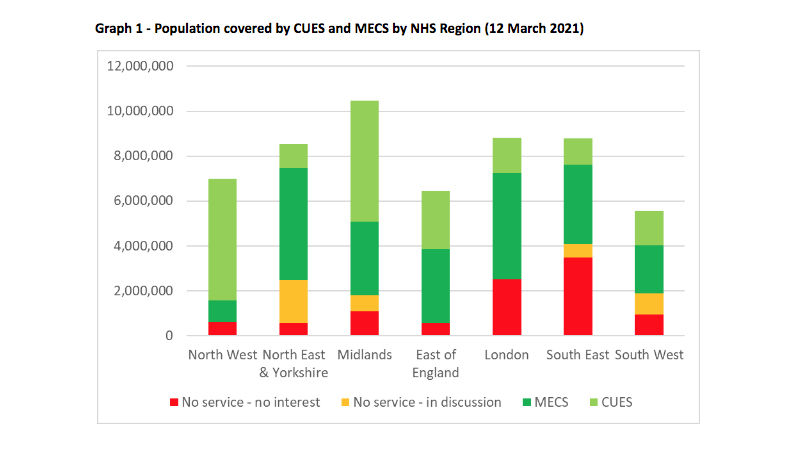
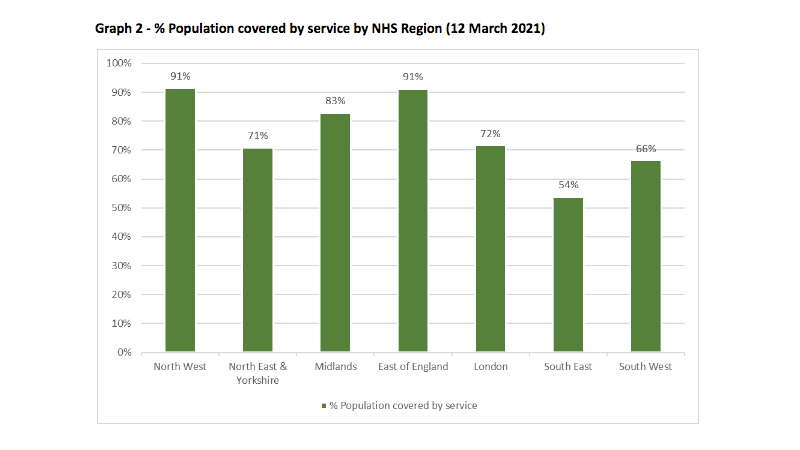
In addition, reports are available for each NHS region, breaking the data down further to ICS level, providing the local commissioning detail.
CUES – Regional Report East of England.pdf
CUES – Regional Report London.pdf
CUES – Regional Report Midlands.pdf
CUES – Regional Report North East and Yorkshire.pdf
CUES – Regional Report North West.pdf

